Compliance Overview - ERISA Compliance FAQs
The Employee Retirement Income Security Act of 1974 (ERISA) is a federal law that sets minimum standards for employee benefit plans maintained by private-sector employers. ERISA includes requirements for both retirement
plans (for example, 401(k) plans) and welfare benefit plans (for example, group health plans). ERISA has been amended many times over the years, expanding the protections available to welfare benefit plan participants and
beneficiaries.
The Department of Labor (DOL), through its Employee Benefits Security Administration (EBSA), enforces most of ERISA’s provisions. Violating ERISA can have serious and costly consequences for employers that sponsor welfare
benefit plans, either through DOL enforcement actions and penalty assessments or through participant lawsuits.
This Compliance Overview includes a set of frequently asked questions (FAQs) to help employers understand ERISA’s requirements for reporting and disclosure.
Plan Document/SPD
- Employee benefits that are subject to ERISA must be described in a plan document and SPD.
- When a plan is insured, a “wrap document” is used to describe plan benefits.
- Not having a plan document means that the plan is out of compliance with ERISA and the employer will be subject to penalties and fines by the department of labor.
Form 5500
- ERISA-covered employee benefit plans must file a Form 5500 each year, unless an exemption applies.
- Small welfare plans that are unfunded or insured are exempt.
- To qualify for the small plan exemption, the plan must have fewer than 100 covered participants at the beginning of the plan year.
LINKS AND RESOURCES
- The DOL’s Reporting and Disclosure Guide for Employee Benefit Plans
- Form 5500 Series website, which includes links to the Form 5500 and instructions
- FAQs on the Delinquent Filer Voluntary Compliance Program
Need to reference a compliance calendar? Download the following document to be sure you don't miss any dates!
Plan Document
Does Every ERISA Plan Need a Written Plan Document?
Yes. If an employer decides to provide benefits that are subject to ERISA, those benefits must be described in a written plan document. The plan document describes the terms of the plan and the plan’s operation and administration. An ERISA plan may exist without a plan document—not having a plan document just means that the plan is out of compliance with ERISA.
Which Topics Must the Plan Document Address?
There are several topics that must be addressed in the written plan document for a welfare benefit plan. For example, the plan document should address:
✓ Benefits and eligibility;
✓ Funding of benefits;
✓ Treatment of insurance refunds and rebates;
✓ Procedures for claims and appeals;
✓ Designation of named fiduciary;
✓ Plan amendment and termination procedures;
✓ Required provisions for group health plans, such as COBRA rights and HIPAA special enrollment;
✓ Other legal provisions applicable to certain plans (such as subrogation and reimbursement and coordination of benefits); and
✓ Procedures for allocating and delegating plan responsibilities (for example, where certain administrative tasks will be performed by a third-party administrator, or TPA).
What Should the Plan Document Look Like?
ERISA does not require that a plan document be in any particular format. The type of plan document depends mainly on the type of plan and the complexity of its benefits. When an ERISA plan is insured, the insurance company’s insurance certificate will often contain detailed benefit information. However, in most cases, the insurance certificate will not contain all of the provisions required for an ERISA plan document. For example, while the certificate may contain a detailed schedule of benefits, it may not address plan amendment and termination procedures.
The standard way of supplementing the certificate is to use a “wrap document” that contains the missing ERISA provisions. This document is called a “wrap document” because it essentially wraps around the certificate to fill in the missing provisions and becomes a single ERISA plan document.
Can Multiple Welfare Benefits Be Combined Into a Single Plan?
Yes. An employer may choose to combine its welfare benefits under a single plan document, creating one large “bundled” plan. An employer may also choose to include certain non-ERISA benefits, such as the Section 125 plan and dependent care FSA, in a bundled plan. Alternatively, an employer may choose to group its benefits into more than one ERISA plan.
The decision of whether to combine (or bundle) welfare benefits often depends on
how it will affect the Form 5500 filing obligation.
- For larger employers, combining different benefits together may simplify the annual reporting requirement because only one Form 5500 will be required for the bundled plan.
- For smaller employers, however, each benefit offered as a separate plan may qualify for the Form 5500 exemption for small plans. Combining the benefits together under a bundled plan might cause the plan to exceed the threshold for small plans, which would trigger the Form 5500 filing requirement.
The standard method for combining different benefits in a bundled plan is to use a wrap plan document. This document would wrap around all the documents (for example, insurance certificates or documents prepared by TPAs) to include the missing ERISA provisions and combine the benefits into one plan. This document is sometimes referred to as a “mega wrap document” because it covers multiple welfare benefits.
Summary Plan Description
What Is a Summary Plan Description (or SPD)?
An SPD is a document that is provided to plan participants to explain their rights and benefits under the welfare benefit plan. The SPD must be written in a manner calculated to be understood by the average plan participant. ERISA and DOL regulations require SPDs to include certain types of information, such as information to help participants identify their plan. There are also requirements for when and how the SPD must be distributed to participants.
SPDs are important documents under ERISA, and they should be carefully prepared and reviewed. When there is a discrepancy between the plan document and the SPD, courts have often ruled that the SPD’s terms will be enforced if they are more beneficial to the plan’s participants.
Are all Welfare Benefit Plans Required to Provide Participants with an SPD?
Virtually all welfare benefit plans subject to ERISA must provide participants with an SPD, regardless of size. Both insured and self-funded group health plans must comply with ERISA’s SPD requirements. While ERISA contains an exception for certain welfare benefit plans with fewer than 100 plan participants, that exception only applies to the Form 5500 filing requirement, and does not apply to SPDs.
Who Is Responsible for Providing the SPD?
Under ERISA, the plan administrator is legally responsible for making sure the SPD is provided, not the insurer or a TPA. This is generally true even if another company is contractually obligated to help draft the SPD. The plan administrator is the entity designated under the terms of the plan. For single-employer ERISA plans, the plan administrator is the employer that sponsors the plan, unless the plan document designates a different entity.
Which Topics Must the SPD Address?
ERISA provides detailed content requirements for welfare benefit plan SPDs. Under ERISA, the SPD must address the following topics related to the plan:
✓ Plan identifying information;
✓ Benefits and eligibility rules;
✓ Circumstances causing loss or denial of benefits;
✓ Plan amendment, termination and subrogation provisions;
✓ Contributions and funding;
✓ Claims procedures;
✓ Statement of ERISA rights;
✓ Additional group health plans requirements; and
✓ Prominent offer of assistance in a non-English language (if required).
Does the Certificate or Booklet Prepared by the Insurer or TPA Qualify as an SPD?
Some plan sponsors mistakenly believe that providing participants with the booklet issued by the insurance company or TPA fulfills their obligation to provide participants with an SPD. This booklet, or certificate, will often contain detailed information regarding plan benefits and coverage. However, in most cases, the booklet prepared by the insurer or TPA will not include all the information that must be included in an SPD.
As a solution, plan sponsors can create a separate document, often called a “wrap SPD” that includes the ERISA-required information that the booklet prepared by the insurer or TPA does not include. In this scenario, the wrap SPD and the booklet, together, make up the plan’s SPD.
What Are the Deadlines for Providing the SPD?
Participants must receive an SPD:
- Within 120 days of the plan becoming subject to ERISA (for example, a new group health plan);
- Within 90 days of enrollment for new participants; and
- Within 30 days of a participant’s written request for an SPD.
In addition, an updated SPD must be provided to participants at least every five years, if material modifications have been made during that period. If no material modifications have been made, an updated SPD must be provided at least every 10 years. As a practical matter, to help participants understand their plan benefits, plan administrators should provide new participants with SPDs and distribute updated SPD information to current participants as soon as possible.
When Must Changes to the SPD Be Communicated to Plan Participants?
A summary of material modification (SMM) must be provided when there is a material modification in the terms of the plan or any change in the information required to be in the SPD. The SMM updates the plan’s SPD. Thus, a plan’s SPD will include all the SMMs that have been provided, but not yet incorporated into the SPD document.
As a general rule, the plan administrator must provide the SMM within 210 days after the close of the plan year in which the change was adopted. A shorter deadline may apply in some circumstances, depending on the nature of the modification or change. If the change is a material reduction in group health plan benefits or services, the deadline for providing the SMM is 60 days after the change is adopted.
In addition to the SPD, the Affordable Care Act (ACA) requires plan administrators and issuers to provide participants with a summary of benefits and coverage (SBC). Plan administrators and issuers must provide 60 days’ advance notice of any material modification to plan terms or coverage that takes effect mid-plan year and affects the content of the SBC. The 60-day notice can be provided to participants through an updated SBC or by issuing an SMM.
How Should SPDs Be Distributed to Participants?
The plan administrator is required to provide the SPD to participants in a manner reasonably calculated to ensure actual receipt of the material by the participant. The following are examples of acceptable methods of delivery:
- In-hand delivery to employees at their worksite (merely posting information in a common area is not acceptable)
- Included within a periodical distributed to employees (for example, a union newsletter or company publication)
- U.S. mail
- Electronic media (DOL regulations include a safe harbor provision applicable to electronic delivery of SPDs)
Does ERISA Require That SPDs Be Provided In A Language Other Than English?
No. While ERISA does not require that an SPD be provided in a non-English language, in some cases the SPD must include a prominently displayed notice that assistance in a non-English language is available. Whether a plan must provide language assistance depends on the size of the plan and the percentage of plan participants who are literate only in the same non-English language, as follows:
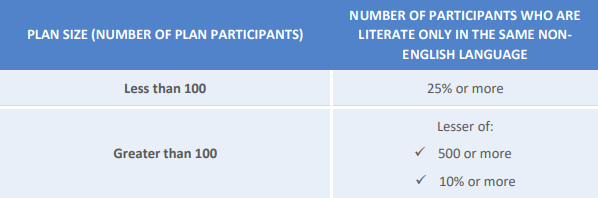 Example: An employer maintains a group health plan that covers 1,000 plan participants. At the beginning of the plan year 500 participants are literate only in Spanish, 101 are literate only in Vietnamese, and the remaining are literate in English.
Example: An employer maintains a group health plan that covers 1,000 plan participants. At the beginning of the plan year 500 participants are literate only in Spanish, 101 are literate only in Vietnamese, and the remaining are literate in English.
Each of the 1,000 plan participants must receive an SPD that contains a notice in both Spanish and Vietnamese explaining the ability to obtain assistance with understanding the SPD.
What Are the Penalties for Not Having a Written Plan Document/SPD?
There are no specific penalties under ERISA for failing to have a plan document or SPD. However, not having a plan document or SPD can have serious consequences for an employer, including the following:
- Inability to Respond to Participant Requests: The plan document/SPD must be furnished in response to a participant's written request. The plan administrator may be charged up to $110 per day if it does not provide the plan document within 30 days after an individual's request. These penalties may apply even where a plan
document/SPD does not exist. - Benefit Lawsuits: Not having a plan document may put an employer at a disadvantage in the event a participant
brings a lawsuit for benefits under the plan. Without a plan document, it will be difficult for a plan administrator
to prove that the plan’s terms support benefit decisions. Also, without a plan document, plan participants can use past practice or other evidence outside of the actual plan’s terms to support their claims. Additionally, courts will likely apply a standard of review that is less favorable to the employer (and more favorable to participants) when reviewing benefit claims under an unwritten plan. - DOL Audits and Requests: The DOL has broad authority to investigate or audit an employee benefit plan’s
compliance with the ERISA. When the DOL selects an employer’s health plan for audit, it will almost always ask to see a copy of the plan document and SPD, in addition to other plan-related documents. If an employer cannot
respond to the DOL’s document requests, it may trigger additional document requests, interviews, on-site visits or even DOL enforcement actions. Also, the DOL may charge a plan administrator up to $161 per day (up to a maximum of $1,613 per request) if it does not provide plan documentation to the DOL upon request.
Participant Requests for Documents
Are ERISA Plans Required to Respond to Participants’ Requests for Documents?
Yes. In addition to the SPD and SBC, which are provided to participants automatically, a plan administrator must provide certain documents upon written request by a participant or a beneficiary. For example, upon written request, the plan administrator must provide the latest SPD, SMMs, and annual report (or Form 5500 for the plan).
The plan administrator must also provide a copy of any bargaining agreement related to the plan, any trust agreement, and any contract or other instrument under which the plan is established or operated. In addition to providing certain documents on request, a plan administrator must make copies of these documents available for examination by any participant. The copies must be provided within 30 days of receiving the written request. The plan administrator may impose a reasonable copying charge for the documents.
Annual Report – Form 5500
Which Welfare Benefit Plans Are Subject to the Form 5500 Requirement?
Administrators of ERISA-covered welfare benefit plans are required to file an annual Form 5500, unless a reporting exemption applies. Whether a plan qualifies for a full or partial exemption from the Form 5500 filing requirement depends on the plan’s size and funding.
Full exemption for certain small plans
Small welfare plans are completely exempt from the Form 5500 filing requirement if they:
• Have fewer than 100 covered participants at the beginning of the plan year; and
• Are unfunded (benefits are paid from the employer’s general assets) or are insured.
The plan can have a combination of insured and unfunded benefits and still qualify for
the exemption.
Partial exemption for certain large plans
Large welfare plans are not exempt from the Form 5500 filing requirement, but they are not
required to comply with all of the Form 5500 filing requirements. This limited filing exemption
applies only if the plan is unfunded, insured, or a combination of unfunded and insured. Plans
that qualify for this exception are not required to file Schedule H, which focuses on the plan’s
financial information, and they are not required to file an accountant’s opinion.
Who Are Covered Participants?
Participants are covered by the plan on the earlier of:
• The date the plan says participation begins;
• The date the individual becomes eligible to receive a benefit; or
• The date the individual makes a voluntary or mandatory payment.
Participants may include employees and former employees (for example, COBRA beneficiaries). However, covered
dependents are not counted as participants.
What Is the Deadline for Filing Form 5500?
The Form 5500 must be filed by the last day of the seventh month following the end of the plan year, unless an extension applies. For calendar year plans, the deadline is normally July 31 of the following year.
A plan administrator may request a one-time extension of two and one-half months by filing IRS Form 5558 by the
un-extended due date of the Form 5500. If the Form 5558 is filed on or before the normal due date of the Form 5500 or 5500-SF, the extension is automatically granted. In addition, an automatic extension for filing Form 5500 until the due date of the employer’s federal income tax return will apply if:
• The plan year and the employer’s tax year are the same;
• The employer has been granted an extension of time for filing its federal income tax return to a date later than the normal due date for the Form 5500; and
• The plan administrator maintains a copy of the application for extending the due date of the employer’s federal
tax return.
This automatic extension cannot be further extended by using Form 5558, and it cannot extend beyond a total of nine and one-half months following the close of the plan year.
How is the Form 5500 Filed with the DOL?
The Form 5500, including required schedules and attachments, must be filed electronically using the DOL’s EFAST2 electronic filing system. Administrators cannot file paper annual reports by mail or other delivery service. Under EFAST2, plan filers may choose to use either approved third-party vendor software or the DOL’s web-based filing system (IFILE) to prepare and submit Forms 5500.
How Many Forms 5500 Is an Employer Required to File?
For benefits provided by a single business entity, the number of annual reports to file depends on how many separate ERISA plans the plan sponsor maintains. A plan sponsor can determine how many separate ERISA plans it maintains by reviewing its employee benefit plan documents. For plan sponsors that are part of a controlled group, generally only one Form 5500 is required for each employee benefit plan maintained by the controlled group. However, in a controlled group setting, consideration must be given to whether the funds contributed by controlled group members are available to provide benefits to all eligible employees of the controlled group.
Plan sponsors may decide to combine more than one type of ERISA welfare benefit into a single plan to consolidate annual reporting. The intention to combine benefits into a single plan should be reflected in the governing plan documents, such as a wrap document. If ERISA welfare benefits are combined into a single plan, the plan administrator would generally only be required to annually file one Form 5500 for the plan’s benefits.
What Are the Penalties For Not Complying with the Form 5500 Requirements?
The DOL can assess penalties for noncompliance with the annual reporting requirements, including submitting incomplete Forms 5500 or not filing Forms 5500 by the due date. For example, the DOL has the authority under ERISA to assess penalties of up to $2,259 per day for each day an administrator fails or refuses to file a complete Form 5500. The penalties may be waived if the noncompliance was due to reasonable cause. In addition, ERISA provides for criminal penalties for willful violations of its reporting requirements.
What Is the Delinquent Filer Voluntary Compliance Program?
The Delinquent Filer Voluntary Compliance Program (DFVCP) was created by the DOL to encourage employee benefit plan administrators to voluntarily file overdue Forms 5500. The DFVCP gives delinquent plan administrators a way to avoid potentially higher penalty assessments by voluntarily completing their late Form 5500s for a year and paying reduced penalties. Plan administrators are eligible to use the DFVCP only if they make the required filings prior to being notified in writing by the DOL of a failure to file a timely annual report.
Summary Annual Report
What Is the Summary Annual Report?
Plan administrators that are required to file a Form 5500 must provide participants with a summary of the information in the Form 5500, called a Summary Annual Report (SAR). Plans that are exempt from the Form 5500 filing requirement are also exempt from providing the SAR. In addition, unfunded welfare plans, regardless of size, are not required to provide the SAR.
The SAR is required to include certain information, provided that information was required to be included on the plan’s Form 5500. In general, an SAR must include:
• Funding and insurance information;
• Basic financial information; and
• A statement that participants have the right to request a copy of the full annual report
In addition, the SPD requirements regarding foreign language assistance also apply with respect to SARs. The offer of assistance must be written in the non-English language of the participants and must be included with the SAR.
The plan administrator generally must provide the SAR within nine months of the close of the plan year. If an extension of time to file the Form 5500 is obtained, the plan administrator must furnish the SAR within two months after the close of the extension period
Is your business set up with the best approach to compliance? Not sure? Contact WD & Associates to discuss how we can help. You can also save the information in this blog by downloading the PDF here.
This Compliance Overview is not intended to be exhaustive nor should any discussion or opinions be construed
as legal advice. Readers should contact legal counsel for legal advice. ©2014-2019, 2021 Zywave, Inc. All rights
reserved.













Leave a comment